Internal Hemorrhoids: Diagnosis & Endoscopic Treatment
Internal hemorrhoids are swollen veins located deep inside the rectum. While they are often painless in the early stages, they can cause significant discomfort and bleeding as they progress. As a consultant in endoscopic gastrointestinal procedures, I emphasize that an accurate diagnosis is the cornerstone of effective, non-surgical treatment.
What Causes Internal Hemorrhoids ?
Hemorrhoids develop when there is increased pressure in the lower rectum. Common contributing factors include:
Chronic Straining: Often due to constipation or diarrhea.
Sedentary Habits: Prolonged sitting, particularly on the toilet, which weakens rectal support.
Pregnancy & Childbirth: Increased pelvic pressure and hormonal changes.
Lifestyle Factors: Obesity and a low-fiber diet are primary triggers.
Common Symptoms to Watch For
Because internal hemorrhoids are located above the “pain line” in the rectum, they may not cause pain initially. Look out for:
- Painless Bleeding: Noticing bright red blood on the tissue or in the bowl after a bowel movement.
- Prolapse: Hemorrhoids that protrude through the anal opening during strain.
- A Feeling of Fullness: A persistent sensation that the bowels are not completely empty.
- Mucus Discharge: Which can lead to localized skin irritation or itching.
Precision Diagnosis via Endoscopy
Clinical examination alone may not reveal the full extent of the condition. In our practice, we utilize advanced diagnostic tools to ensure the highest accuracy:
Anoscopy: A specialized view of the anal canal to identify enlarged veins.
Flexible Sigmoidoscopy: This allows us to examine the lower part of the colon .
Full colonoscopy: This allows us to examine the entire colon, ensuring that bleeding is not caused by other conditions like polyps or inflammation
Quick Facts: Endoscopic Hemorrhoid Treatment
Did you know?
- Procedure Time: Endoscopic banding (RBL) usually takes less than 10 minutes.
Pain Level: Minimal to none, as internal hemorrhoids are in a non-sensitive zone.
Recovery: Most patients return to normal activities within 1 hour.
Success Rate: Over 90% of patients see significant improvement without surgery.
Key Advantage: No general anesthesia or hospital stay is required.
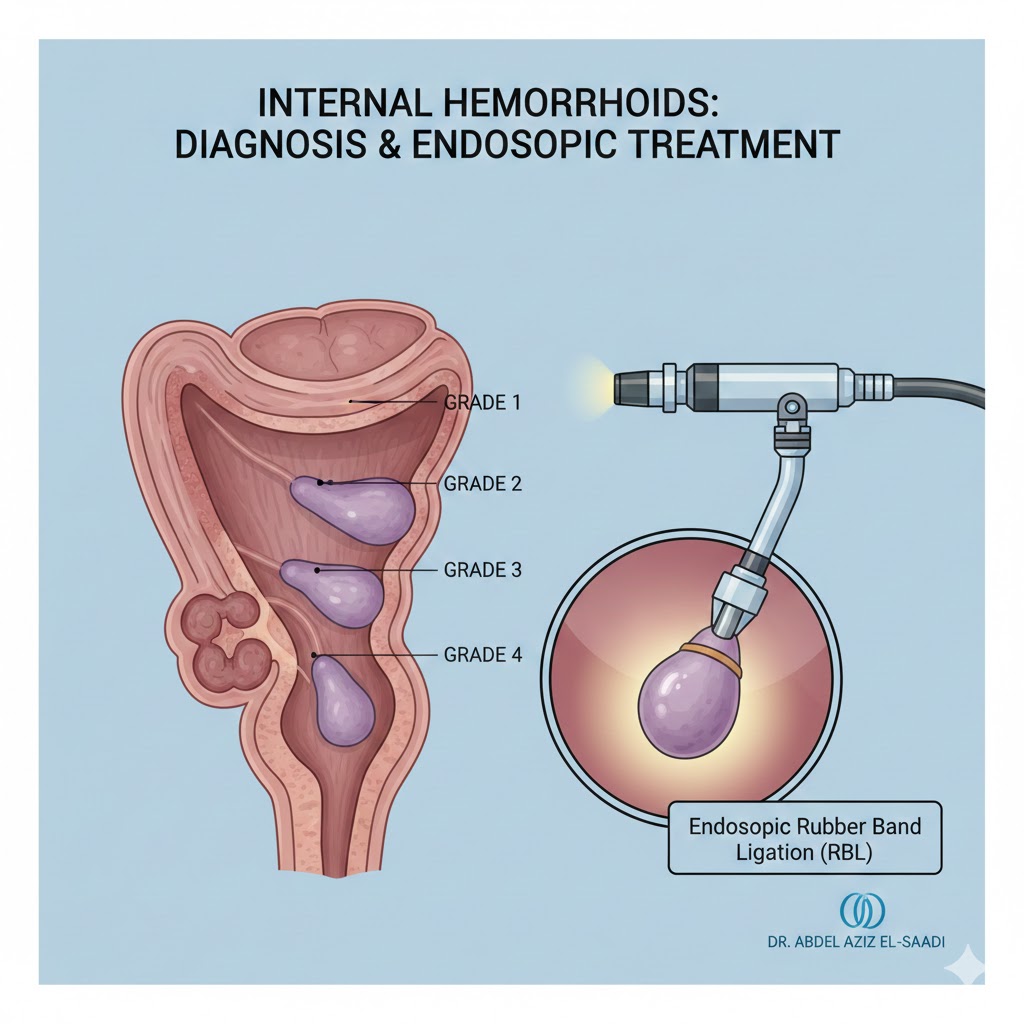
Why Endoscopy?
It allows for “grading” the hemorrhoids (Grade I to IV), which is essential for determining whether a patient needs simple lifestyle changes or a clinical procedure.
Treatment Pathways: From Prevention to Procedure
Our goal is always to resolve symptoms using the least invasive methods possible.
1. Lifestyle & Conservative Management
- Fiber-Rich Diet: Incorporating whole grains, fruits, and vegetables.
- Hydration: Ensuring adequate water intake to soften stools.
- Physical Activity: Helping to regulate bowel movements.
2. Specialized Endoscopic Treatments (Non-Surgical)
For persistent cases, we offer highly effective, in-office procedures:
- Rubber Band Ligation: The “Gold Standard” for internal hemorrhoids, where a small band is applied to cut off blood flow to the hemorrhoid.
3. Surgical Intervention
Reserved only for advanced, treatment-resistant cases (Grade IV) where other methods are no longer viable.
Doctor’s Note:
Early diagnosis through endoscopy can prevent the need for surgery. If you are experiencing rectal bleeding, it is vital to seek a professional evaluation to rule out other gastrointestinal issues.
End the discomfort today. Get a precise diagnosis and start your non-surgical recovery now.
